No products in the cart.
Oradix Stemdetox – Methyl B’s, 50+ ingredients – Professional detoxification
5 out of 5 based on 1 customer rating
(1 customer review)
100% of buyers said they were satisfied.
$132.00 $113.00
A professional strength, advanced detoxification, antioxidant, anti-biofilm, natural anti-bacterial, antiviral, anti-fungal, plus supports the gut, the lymph and longevity
Out of stock
Product Description
StemDetox™ Methylated Advanced – 8th generation, with 50+ ingredients, 150 capsules
(without Iron, Iodine or Copper)
A professional strength, advanced detoxification, antioxidant, anti-biofilm, natural anti-bacterial, antiviral, anti-fungal product, plus supports the gut, the lymph system, and longevity and excellent in supporting fasting and ketogenic diet.
Save over $300 compared to buying the ingredients alone or in small groups.
The painstakingly balanced ingredients might be compared to a world-class orchestra where all of the ‘musical instruments’ express the highest level of art, rarely encountered in music or in superb wellness.
In fact, StemDetox stands alone. Like the tallest tree on Earth.
There is no other product like StemDetox. None.
StemDetox™ favored in:
- immune boosting;
- raising glutathione levels;
- anti-biofilm;
- excellent companion in ketogenic diet;
- overnight detoxification is extended in intermittent fasting or regular fasting – StemDetox supports with balance (supporting lymph, liver, kidneys, microcirculation, etc.) detoxification and increased mineral needs in fasting;
- leaky gut;
- cold and flu (including swine-flu or bird-flu);
- acne;
- prostate enlargement and prostate cancer support;
- breast cyst and breast cancer;
- age-spots on the skin;
- tiredness;
- parasites;
- Candida;
- infections caused by ‘multi-resistance’ bugs (together with EDTA containing products, such as EDTA line- 2.0, 1.0, 0.5 or ToxDetox as EDTA enhances antibacterial action);
- toxic heavy metal removal (less effective than the EDTA line, but nicely supports the removal of toxins, – based on small research study when 36 urine samples were collected and analyzed);
- most important ‘natural emergency product’ kept in the kitchen for uncertain times;
- removal of scar tissues due to its high level of ‘systemic enzyme’ Serrapeptase;
- support (and more) for diabetics;
- replaces minerals in chelation programs;
- real anti-aging when synergistic toxins and synergistic microbes are targeted;
- and others…
The latest StemDetox surpasses the previous versions in quality and effectiveness with the added EDTA and vitamin C and more.
StemDetox is the first supplement that was also developed to detoxify the bone marrow.
Other stem cell enhancing products ‘force’ the bone marrow to release more stem cells, even if the bone marrow is weak and loaded with toxins.
Our approach and philosophy are different.
Let’s detoxify the bone marrow for the production of more and healthier stem cells. Over time a healthier, detoxified bone marrow ensures the raised stem cell baseline numbers in the blood. This is a novel concept and we’re still the only ones out there to promote this life-changing idea.
StemDetox is a one-of-a-kind product resulting in huge savings (over $300 saved) compared to buying the ingredients individually or in smaller groups.
Proper detoxification slows down the rate of aging on a cellular level and lowers the risk for all diseases
StemDetox establishes a new category among the detoxification / cleansing products with its antibacterial, antiviral, anti-fungal, anti-parasitic, circulatory support and weight-loss properties. StemDetox is innovative, safe and effective and transforms detoxification as we know it today.
StemDetox achieves full-body cellular detoxification and overall cleansing by aiding the seven channels of elimination: the liver, lungs, colon, kidneys, blood, skin, and lymphatic system. It also supports the two phases of the liver’s complex detoxification mechanisms (Phase I and II).
Highly toxic mercury and lead inhibit the key white blood enzyme myeloperoxidase, an enzyme that produces hypochlorite ion. Since this is the body’s main defense against Candida yeast(1), it is difficult to solve Candida yeast problems unless the toxic metals are removed first. StemDetox not only eliminates heavy metals but also has the strongest natural anti-fungal ingredients (garlic, caprylic acid, grapefruit seed extract, oil of oregano, serrapeptase). Most people want to lower their toxic heavy metal load for improved heart and circulatory benefits or to avoid bypass surgery. However, a Swiss study showed the cancer preventative effects by concluding that those who removed the toxic metals achieved a 90% reduction in cancer mortality over an 18 years period(2).
StemDetox is the first detoxification product that contains a systemic, proteolytic enzyme ingredient (Serrapeptase). Systemic (proteolytic) enzymes can enhance detoxification and reduce inflammation and swelling, digest scar tissues, blood clots and cysts, improve varicose veins and arthritis, guard against fibrosis and improve fibrocystic breast disease, modulate the immune system, block the release of pain in inflamed tissues and even fight off viruses or turn around Type 1 diabetes(3). Enzymes also increase the effectiveness of other ingredients, allowing a lower dose to have superior results. This makes StemDetox highly efficient. Systemic enzymes also reduce the occasionally experienced die-off (Herxheimer reactions).
Even if a great detoxification protocol is followed, large amounts of fat-soluble toxins remain in the fat cells, unless weight-loss is concurrent with detoxification. People often get sick when they lose weight because they flood their body with newly released toxins from within the body. StemDetox is the first and only product on the market that opens up fat cells while actively eliminating toxins from the body, resulting in weight-loss.
StemDetox has many benefits for those who are on a ketogenic diet. In an effective keto diet or ketogenic diet, less than 5% of calories come from carbohydrates (including sugar), over 80% of calories come from good fats (avocado, coconut oil, nuts and nut butter, olive oil, chia seeds and flex seed). I love eating for a healthy lunch an avocado and a sliced apple with almond nut spread on the slices. Avoid trans fats always, found in margarine, store-bought cookies, crackers, cakes and frozen pizza.
StemDetox supports the extra effort of the heart and circulatory system. Naturally, full-body detoxification requires the opening up of the capillaries (tiny blood vessels) for a profound, cellular detoxification. Otherwise, areas of the body with poor circulation couldn’t be detoxified. StemDetox is the first detoxification product that enhances microcirculation.
Another first: StemDetox’s brain protective ingredients have important synergistic effects to guard the brain against neurotoxins that might be elevated at any detoxification.
Detoxification requires extra energy, and StemDetox is the first detoxification product that has energy boosting ingredients to aid the mitochondria, the energy-producing centers of cells.
Detoxification is more effective if disease-causing agents (bacteria, viruses, yeast, and parasites) don’t burden the body. StemDetox contains antibacterial, antiviral, anti-fungal and anti-parasitic ingredients. Since parasites have the potential to store large amounts of toxins, their elimination reduces the overall toxic load.
It is a well-known fact that stomach ulcers are caused by a bacterium called Helicobacter pylori. But it’s not widely known that Chlamydia pneumoniae, has recently been linked to heart disease. Doctors are consistently finding the same Chlamydia in arterial plaque removed from coronary arteries(4).
Furthermore, researchers found the same Chlamydia bacterium in the autopsied brains of seventeen out of nineteen Alzheimer’s patients(5).
Recent research verified the link between hepatitis B and C and liver cancer, and studies have confirmed that herpesvirus 8 is the cause of Kaposi’s sarcoma (another type of cancer)(6).
Moreover, population studies point out the so far unexplained sudden spread of MS in regions where there were no previous cases(7).
Even the ‘incurable’ Chron’s disease is now associated with a yeast, Saccharomyces cerevisiae(8).
Type 2 diabetes responds strongly to the four anti-fungal approaches: the removal of toxic heavy metals; the reduction (or elimination) of sugar (fungus strives on sugar); reduction or elimination of wheat in the diet (there is extremely toxic fungal aflatoxin in wheat); and to anti-fungal products(9), plus overall caloric restriction and regular exercise are paramount for diabetics. Not much change can be expected for stopping diabetes without losing weight and exercising.
Throughout history, more people have died of infectious diseases than from any other cause. According to the ‘New Germ Theory’, the leading cause of death worldwide continues to be infectious diseases such as heart disease, Alzheimer’s, herpes, diabetes and MS (although mainstream medicine does not openly discuss new medical discoveries(10). StemDetox is the first and only detoxification / cleansing product that recognizes the key role infectious agents play in chronic diseases.
You Can Change Your Lifestyle
As you detoxify, drink more filtered water than usual for better elimination of toxins. Eat healthy foods and eat more raw fruits and vegetables, preferably organic. Take your daily multivitamins, multiminerals, omega 3 oils, and probiotics (or ‘organic’ bio-yoghurt). The beneficial Lactobacillus bacterium is very important to replenish the bacterial flora in the gut. Keep your blood sugar level low by reducing sugar and wheat in your diet. Eat less than what you desire since calorie restricted diet is one of the best way to slow down aging. Avoid red meat and trans-fat. Keep your healthy weight. Don’t forget the basics: your daily exercise and 7-8 hours sleep. Detoxification should be extended into your whole life since body, mental and spiritual health are inherently linked. Detoxify your visual input by watching less TV and by avoiding violent movies (which can depress your immune system). Reach out to others who are less fortunate. Pick up a new hobby that would enrich your life. Love more and forgive those who hurt you(11). Meditate and say your daily prayers. Be thankful for what you have. Go out to nature and marvel at the beauty of our world.
For more info, visit: www.StemDetox.com
These statements have not been evaluated by the US FDA. This product in not intended to diagnose, treat, cure or prevent any disease. As with any dietary supplement, consult your doctor before using natural health products or change your lifestyle.
References:
[1] Shaw, Dr. William. Biological Treatments for Autism and PDD. Chapter 8. The Great Plains Laboratory, 2002.
[2] Walter Blumer, M.D. and Elmer Cranton, M.D., Ninety Percent Reduction in Cancer Mortality After EDTA Chelation, Journal of Advancement in Medicine, Vol.2, Num.1/2, Spring/Summer 1989.
[3] Woche, Medizinische. Systemic Enzyme Therapy. Baden Baden, Germany, Oct. 27-Nov. 4, 1990.
[4] Campbell, LA. Kuo, CC. Chlamydia Pneumoniae and Atherosclerosis. Semin Respir Infect. 2003 Mar; 18( 1): 48-54.
[5] Balin BJ et all., Chlamydophila pneumoniae and the etiology of late-onset Alzheimer’s disease. J Alzheimers Dis. 2008 May; 13( 4): 371-80.
[6] Schwartz RA, Micali G, Nasca MR, Scuderi L., Kaposi sarcoma: a continuing conundrum. J Am Acad Dermatol. 2008 Aug; 59( 2): 179-206; quiz 207-8.
[7] Vázquez MC et all, Incidence and prevalence of amyotrophic lateral sclerosis in Uruguay: a population-based study. Neuroepidemiology. 2008; 30( 2): 105-11. Epub 2008 Mar 11.
[8] McKensie H et al. Antigenic heterogeneity of strains of Saccharomyces cerevisiae and Candida albicans recognized by serum antibodies from patients with Crohn’s disease. FEMS Microbio. Immunol 89:219-224, 1992.
[9] Kaufman, AK., Infectious Diabetes, Mediatrition, 2003.
[10] A New Germ Theory, by Judith Hooper, The Atlantic Monthly, Feb 1999
[11] Dr. Gyorgy Irmey, MD; Unexplained sudden healings were experienced by more than 30% of late-stage cancer patients when they offered and received forgiveness at a private cancer clinic in Heidelberg, Germany. (personal communication with Dr. Janossy)
[12] P A S Theophilus et al., Effectiveness of Stevia Rebaudiana Whole Leaf Extract Against the Various Morphological Forms of Borrelia Burgdorferi in Vitro Eur J Microbiol Immunol (Bp). 2015 Dec ;5(4):268-80. Epub 2015 Nov 12. PMID: 26716015
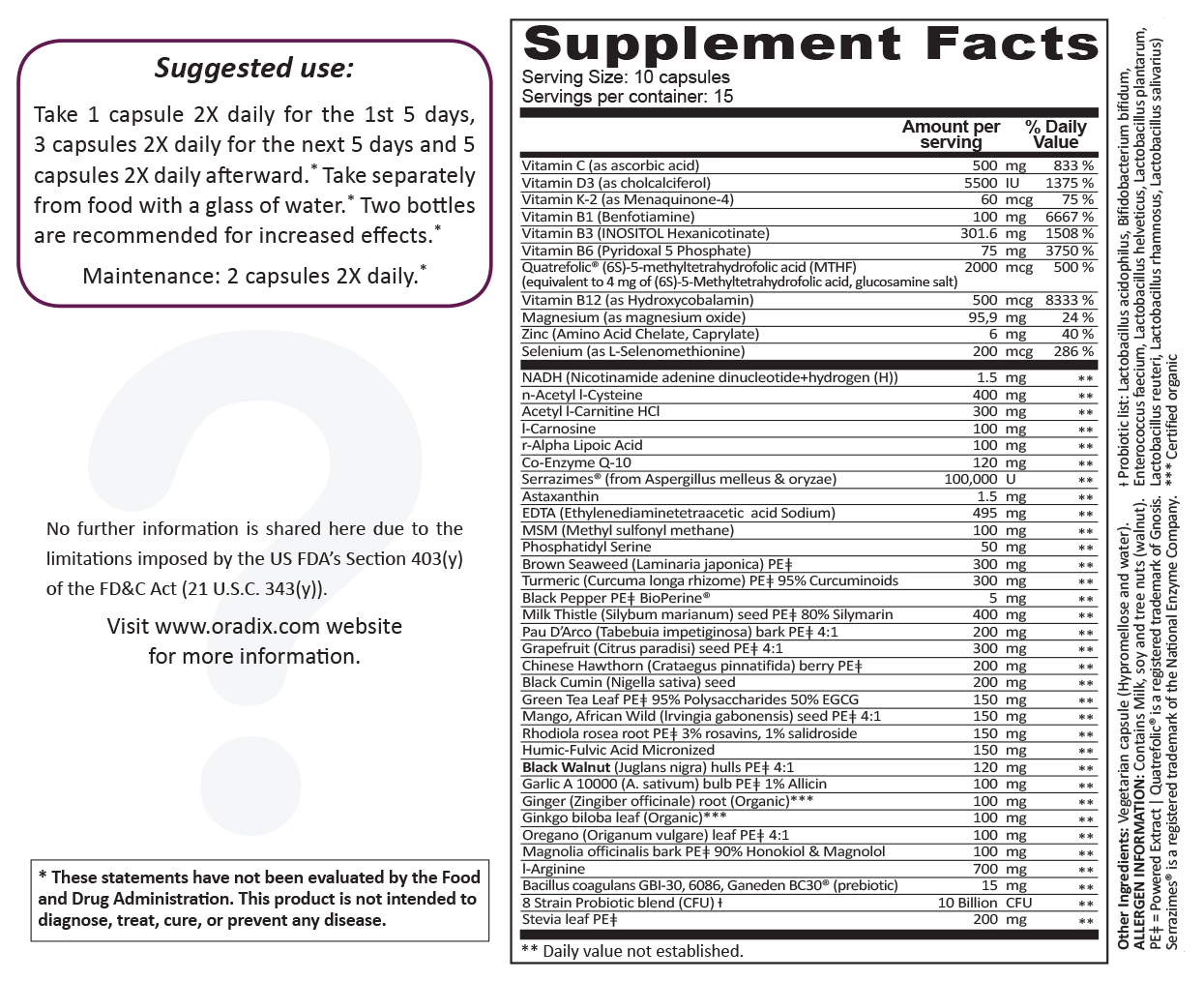
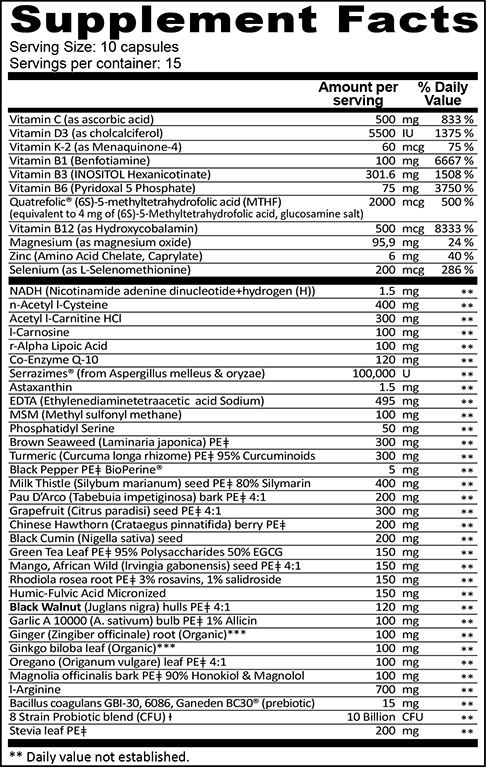
Nutritional Facts and Dosage
How to Use StemDetox™
Take 1 capsule 2X daily for the 1st 5 days, 3 capsules 2X daily for the next 5 days and 5 capsules 2X daily afterward. Take separately from food with a glass of water. Two bottles are recommended for increased effects.
Unpleasant die-off symptoms (Herxheimer reactions) at the beginning of detoxification, such as flu-like symptoms, headache, and tiredness are rarely experienced. However, if they do occur, reduce the number of capsules taken daily or take a break for a day or two and increase the number of capsules again at a comfortable level. Consumption of extra water, systemic enzymes and (powdered) charcoal (StopReabsorb) can all reduce any die-off symptoms.
Maintenance: 2 capsules 2X daily
50+ ingredients — 150 capsules
NEW ingredients in StemDetox™, 8th generation
- EDTA (1st product to have EDTA with other ‘detox’ ingredients) added for detoxifying the gut wall towards the lumen of the gut and also for its anti-biofilm/anti-Candida effects, plus to capture toxins in the gut from the food (only 5% of EDTA is absorbed from the gut, 95% stays in the gut)
- Methylated B vitamins
- Vitamin B12
- Vitamin C
- MSM
- Curcumin
- Black Pepper
- Black Cumin
- Magnolia
- L-Arginine
- Stevia for its strong anti-biofilm effects(12)
- Pre-Biotic (the 1st product to have pre-biotic in a detox product to support the gut microbiome)
- Pro-Biotics (the 1st product to repopulate the gut with good bacteria at the time of detoxification)
Each serving (10 capsules, taken two times 5 capsules between meals) provide:
- Vitamin D3 (Cholecalciferol) — 5,500 IU
- Vitamin K-2 (as Menaquinone-44) — 60 mcg
- Vitamin B1 (Benfotiamine) — 100 mg
- Vitamin B3 (Inositol Hexanicotinate) — 301.6 mg
- Vitamin B6 (pyridoxal 5 phosphate) — 75 mg
- Vitamin B12 (Hydroxycobalamin) — 1 mg
- Ascorbic Acid — 500mg
- Magnesium (as magnesium oxide) — 95.9 mg
- Zinc Caprylate (Amino Acid Chelate) — 6 mg
- Selenium (L-Selenomethionine) — 200 mcg
- NADH (Nicotinamide adenine dinucleotide+hydrogen) — 1.5 mg
- N-Acetyl-L-Cysteine — 400 mg
- Acetyl-L-Carnitine HCL — 300 mg
- l-Carnosine — 100 mg
- R-Alpha Lipoic Acid Sodium Salt — 100 mg
- Co Enzim Q-10 (Ubiquine) — 120 mg
- Serrapeptase (Serrazimes) — 100,000 IU
- Astaxanthin — 1.5 mg
- EDTA Sodium — 495 mg
- MSM — 100 mg
- Phosphatidyl Serine — 50 mg
- Brown Seaweed (Laminaria Japonica) PE — 300 mg
- Curcumin C3 (Curcuma Longa) root PE 95% — 300 mg
- Bioperine Black Pepper PE — 5 mg
- Milk Thistle (S. Marianum) Seed PE 80% Silymarin — 400 mg
- Pau D’Arco (Tabebula impetiginosa) Bark PE 4:1 — 200 mg
- Grape Fruit (Citrus paradisi) seeds PE 4:1 — 300 mg
- Hawthorn (C. pinnatifida) Berry 2% Vitexin — 200 mg
- Black Cumin (Nigella Sativa) seed — 200 mg
- Green Tea Leaf PE 95% Poly 50% EGCG — 150 mg
- Mango African Wild (Irving. Gabonensis) seed PE 4:1 — 150 mg
- Rhodiola Rosea root PE 3% Rosavins, 1% Salidroside — 150 mg
- Humic-Fulvic Acids Micronised — 150 mg
- Black Walnut (Jugians nigra) Hulls PE 4:1 — 120 mg
- Garlic Bulb (A. sativum) PE 1% Allicin — 100 mg
- Ginger (Zinzibe Officinale) Root, Organic — 100 mg
- Gingko Biloba Leaf, Organic — 100 mg
- Oregano (Origano Vulgare) Leaf PE 4:1 — 100 mg
- Magnolia Officinalis bark PE 90% Honokiol and Magnolol — 100 mg
- L-Arginine — 700 mg
- Stevia rebaudiana leaf PE 90% Glycosides — 100 mg
- Ganeden BC 30 (prebiotic) — 7,5 g
- 8 Strain Probiotic blend*** — 5 Billion CFU
***8 Strain Probiotic list: Lactobacillus acidophilus, Bifidobacterium bifidum, Enterococcus faecium, Lactobacillus helveticus, Lactobacillus plantarum, Lactobacillus reuteri, Lactobacillus rhamnosus, Lactobacillus salivarius.
Other Ingredients: Vegetarian capsule (Hypromellose and water).
ALLERGEN INFORMATION: Contains Milk, soy and tree nuts (walnut)
Keep at room temperature or in the fridge. KEEP OUT OF REACH OF CHILDREN. Ask for the advise of your doctor before taking StemDetox™ if you have a medical condition, are currently taking anti-coagulants or are pregnant or breastfeeding.
Save up to 15% on protocol packages
– on top of existing product savings!
15
%
15
%
15
%
$467.00 – $758.00
15
%
15
%
15
%
4.8571428571429 out of 5
$208.00 – $726.00Customer reviews
Rated 5 out of 5 stars
1 reviewAdd a review Cancel reply
Additional Information
| Weight | 0.29 lbs |
|---|---|
| Dimensions | 1.8 × 1.8 × 2.3 in |
Related products
15
%
14
%
15
%
15
%
15
%
4.8571428571429 out of 5
$208.00 – $726.00
21
%
18
%
19
%
$38.00 – $55.00
25
%
4.8888888888889 out of 5
Customers also purchased these products
15
%
15
%
15
%
4.8571428571429 out of 5
$208.00 – $726.00
21
%
Customers also viewed these products
17
%
5 out of 5
14
%
Frequently Purchased Together
14
%
5 out of 5
15
%
15
%
15
%
4.8571428571429 out of 5
$208.00 – $726.00
15
%
15
%
15
%
$467.00 – $758.00
21
%

























1 review for Oradix Stemdetox – Methyl B’s, 50+ ingredients – Professional detoxification